DIANNE GUIANG 1204474
The selection of milliamperage and exposure time, collectively known as mAs directly affects the total quantity of radiation produced during an exposure. Proper mAs selection is one of the most effective ways to yield properly exposed radiographs and reduce patient dose. It is then important to make sure that the amount of time that radiation is being emitted from the x-ray tube matches the time selected by the operator; therefore, it is critical for the exposure timer to be accurate and properly calibrated.
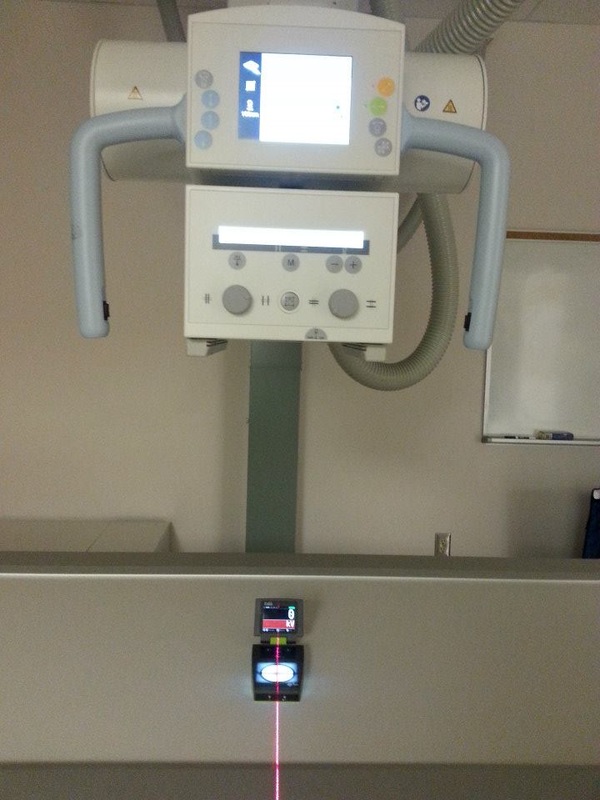
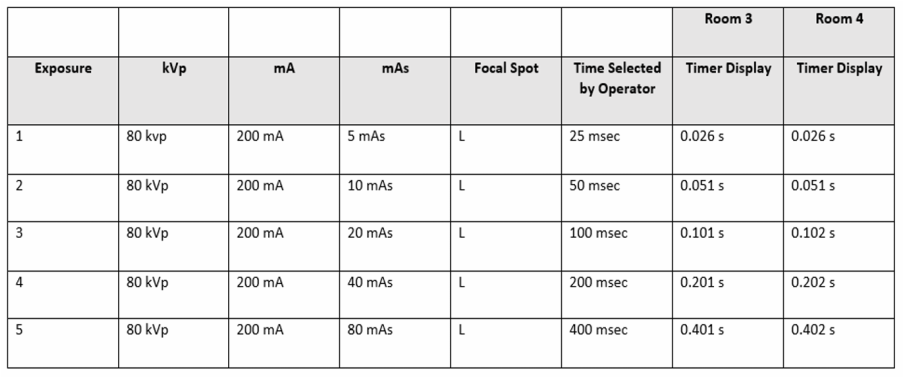
The timer accuracy test was performed to examine the accuracy of the exposure timer in two separate rooms: room 3 and 4 in the B114 lab in the Institute of Applied Health Sciences building. The test was done by exposing a digital timer at a source-to-image distance of 30 inches and a collimation slightly bigger than the exposure area on the digital timer, as can be seen in image 1, 2 and 3. The timer was exposed using the technical factors listed in Table 1 below, and the time displayed by the timer was recorded. Note that two different digital timers were used for each room, both of which were properly calibrated to make sure that both timers were working properly.
The timer accuracy test was performed to examine the accuracy of the exposure timer in two separate rooms: room 3 and 4 in the B114 lab in the Institute of Applied Health Sciences building. The test was done by exposing a digital timer at a source-to-image distance of 30 inches and a collimation slightly bigger than the exposure area on the digital timer, as can be seen in image 1, 2 and 3. The timer was exposed using the technical factors listed in Table 1 below, and the time displayed by the timer was recorded. Note that two different digital timers were used for each room, both of which were properly calibrated to make sure that both timers were working properly.
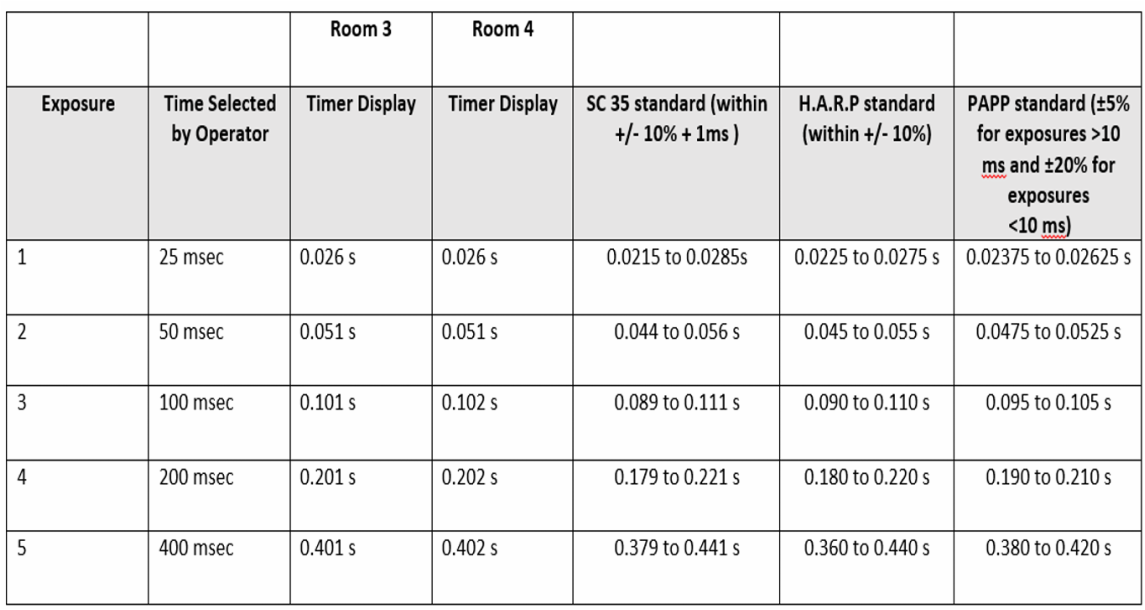
After each exposure, the digital timer displayed the actual length of the exposure. Displayed in Table 2 below is a comparison of the timer display values obtained in this experiment and the values obtained following the standards set by Safety Code 35 (S.C. 35) and the Healing Arts Radiation Protection Act (H.A.R.P).
According to S.C. 35, the actual time of exposure should be within ± 10% + 1 ms of the time selected by the operator. Similarly, according to the H.A.R.P Act, the actual time can deviate from the selected time by no more than ± 10%. Papp (2011) states that exposures >10 ms should be within ±5% and exposures <10 ms can be within ±20%. It can be seen from Table 2 that the results obtained from the timer accuracy tests for rooms 3 and 4 are within the standards set by S.C. 35, H.A.R.P and Papp; therefore, it can be concluded that the timer is accurate and that no corrective action is needed. However, when performing these timer accuracy tests, it is important to make sure that the digital timer is properly calibrated to ensure valid results. Correct selection of technical factors is also important in making sure that the test is performed correctly.
As mentioned before, the accuracy of the timer plays a crucial role in reducing patient dose. An exposure that lasts longer than it should only exposes the patient to unnecessary radiation which results in increased patient dose. An improperly calibrated timer could also cause underexposure (if the duration of exposure is shorter than it should be) and overexposure (if the duration of exposure is longer than it should be) of radiographs. In a digital environment, these problems could be corrected but there can be cases where the resulting radiograph cannot be post-processed into a diagnostically acceptable image. Should problems of underexposure and overexposure arise in a film/screen environment, a repeat x-ray would be absolutely necessary which again increases dose to the patient. Therefore, as outlined in S.C. 35, the irradiation time meter accuracy test should be performed annually to ensure that it is working properly. Also, if the timer is suspected to be malfunctioning, corrective action should be taken immediately. This quality control test allows technologists to apply the ALARA (As low as reasonably achievable) principle effectively and accurately when performing any type of radiographic examination.
As mentioned before, the accuracy of the timer plays a crucial role in reducing patient dose. An exposure that lasts longer than it should only exposes the patient to unnecessary radiation which results in increased patient dose. An improperly calibrated timer could also cause underexposure (if the duration of exposure is shorter than it should be) and overexposure (if the duration of exposure is longer than it should be) of radiographs. In a digital environment, these problems could be corrected but there can be cases where the resulting radiograph cannot be post-processed into a diagnostically acceptable image. Should problems of underexposure and overexposure arise in a film/screen environment, a repeat x-ray would be absolutely necessary which again increases dose to the patient. Therefore, as outlined in S.C. 35, the irradiation time meter accuracy test should be performed annually to ensure that it is working properly. Also, if the timer is suspected to be malfunctioning, corrective action should be taken immediately. This quality control test allows technologists to apply the ALARA (As low as reasonably achievable) principle effectively and accurately when performing any type of radiographic examination.
References
Health Canada. (2008). Safety code 35: Safety procedures for the installation, use and
control of x-ray equipment in large medical radiological facilities.
Retrieved from http://www.hc-sc.gc.ca.
Service Ontario. (2011). Healing Arts Radiation Protection Act.
Retrieved from http://www.e-laws.gov.on.ca/html/regs/english/elaws_regs_900543_e.htm.
Papp, J. (2011). Quality Management in the Imaging Science
(4th ed.). St. Louis, MO: Elsevier Mosby.
control of x-ray equipment in large medical radiological facilities.
Retrieved from http://www.hc-sc.gc.ca.
Service Ontario. (2011). Healing Arts Radiation Protection Act.
Retrieved from http://www.e-laws.gov.on.ca/html/regs/english/elaws_regs_900543_e.htm.
Papp, J. (2011). Quality Management in the Imaging Science
(4th ed.). St. Louis, MO: Elsevier Mosby.